Tag
Directory:
Tags:
|
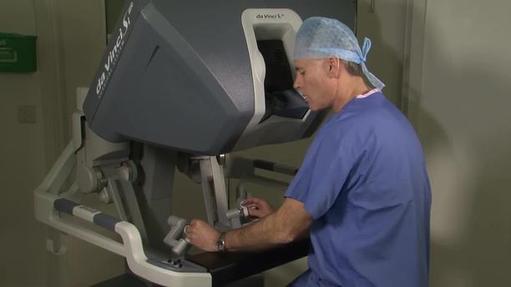
In 2013, a new surgical procedure was used for first time in the UK at St George's Hospital, London to remove of a cancerous kidney tumour.
The procedure combines the da Vinci surgical system with an injection of a dye into the patient's kidney. The dye illuminates healthy tissue and shows up under the da Vinci's camera as a bright green light and as a consequence the procedure is called Firefly. Chris Anderson, a consultant urologist at St George's is one of the early adopters of robotic surgical techniques after receiving specialist training in 2005 at the world renowned Henry Ford Robotic Center in Detroit. Anderson has built-up a leading renal cancer unit at St George's and introduced the Firefly technology into the UK. He says, "Partial kidney removal is a complex operation that requires complete removal of the tumour and reconstruction of the remaining healthy kidney. By combining the da Vinci system with Firefly we are able to achieve our goal better than in the past". Robotic surgery Kidney surgery is enhanced by robotics. In recognition of the increasing importance of high tech surgical therapies, the N Sethia Foundation funded the UK's first robotic surgery training centre at University College Hospital, London. In pride of place in the new Chitra Sethia Centre for Robotics and Minimal Access Surgery is the latest da Vinci surgical system. |
|
|
|
|

Mark Emberton
Honorary Consultant UrologistMark Emberton is Professor of Interventional Oncology in the Division of Surgery and Interventional Science at University College London (UCL). He is also the Clinical Director of the Clinical Effectiveness Unit at the Royal College of Surgeons of England, a Consultant in Urological Oncology at the University College London Hospital, and a member of the Partners’ Council of the National Institute of Clinical Excellence (NICE).
Mark is a world-class expert in prostate cancer who lectures in premier medical institutions throughout the world, and has published more that 200 research papers in peer reviewed journals. He has interests in the design and development of clinical studies, and innovative projects aimed at improving the diagnostic and therapeutic pathways for men with prostate cancer, principally through the use of novel imaging techniques and minimally invasive therapies. Mark leads a research team of clinical innovators that combine knowhow and experience in bioengineering and nanotechnology, and regularly carries out clinical studies aimed at enhancing cancer therapies.
view this profile
Directory:
Tags:

|
Prostate cancer develops in the walnut-sized gland underneath the male bladder. It is the most common cancer, other than skin cancer and is the second leading cause of cancer-related death in men.
The disease, which often develops slowly, is different to most other cancers because small areas of cancer within the prostate are common, especially in older men and may not grow or cause any problems. This presents men diagnosed with prostate cancer with some extremely difficult choices. The statistics Prostate cancer is the second most frequently diagnosed cancer in men and the fifth most common cancer overall. One in six men will be diagnosed with the disease in their lifetime and the overwhelming majority of cases occur in wealthy countries. Each year, about 37,000 men in the UK and some 210,000 men in the US are diagnosed with prostate cancer and more than 10,000 and 28,000 respectively die each year of the disease. In the US there are over two million men living with the disease and African American men have a higher incidence of prostate cancer and double the mortality rate compared with other racial and ethnic groups. In the US about US$10 billion is spent annually on treatments for the disease. Standard treatments Traditional treatments to stop the spread of prostate cancer involve surgery and radiotherapy, which has significant side effects. Following such treatments 50% of patients experience impotence, up to 20% suffer incontinence and between one and five percent who receive radiotherapy experience pain and bleeding. |
|
|

Malcolm Mason
Head of the Oncology and Palliative Medicine Section, Cardiff UniversityProfessor Malcolm Mason is head of the Oncology and Palliative Medicine Section at the School of Medicine. Based at Velindre Hospital, he is also Director of the Wales Cancer Bank. Established in 2003, the Bank is recognised as one of the foremost of its kind worldwide, and has revolutionised opportunities for cancer research, collecting blood and tissue samples from thousands of people in Wales either suffering from cancer or with a potential cancer diagnosis. The Bank is a collaboration involving Cardiff University, the Welsh Assembly Government, the NHS and Cancer Research Wales.
Professor Mason’s own group has carried out a great deal of research into prostate cancer. Through studies which he has led via the MRC, it has been shown that survival rates in men with advanced prostate cancer improve when they are given drugs that preserve bone mass, and more recently that radiotherapy added to hormone therapy reduced deaths from prostate cancer by nearly half in patients with locally advanced disease.
Non-malignant prostate stem cells are known to exist. From their characteristics, it is expected that malignant prostate cancer stem cells will be resistant to hormone treatment and possibly also to chemotherapy and radiotherapy.
Professor Mason said: “We need to know more about prostate cancer stem cells. They could offer new ways to tackle prostate cancer or, at the very least, tell us more about what happens when present treatments fail. We are excited about the opportunities for us to work with the new European Cancer Stem Cell Research Institute to improve our understanding in this particular field.”
view this profile
Directory:
Tags:
Prostate cancer usually doesn't produce any noticeable symptoms in its early stages, so many cases of prostate cancer aren't detected until the cancer has spread beyond the prostate. For most men, prostate cancer is first detected during a routine screening such as a prostate-specific antigen (PSA) test or a digital rectal exam (DRE).
When signs and symptoms do occur, they depend on how advanced the cancer is and how far the cancer has spread.
Less than 5 percent of cases of prostate cancer have urinary problems as the initial symptom. These problems are caused when the prostate tumour presses on the bladder or on the tube that carries urine from the bladder (urethra). However, urinary symptoms are much more commonly caused by benign prostate problems, such as an enlarged prostate (benign prostatic hyperplasia) or prostate infections.
When urinary signs and symptoms do occur, they can include:
- Trouble urinating
- Starting and stopping while urinating
- Decreased force in the stream of urine
Cancer in your prostate or the area around the prostate can cause:
- Blood in your urine
- Blood in your semen
Prostate cancer that has spread to the lymph nodes in your pelvis may cause:
- Swelling in your legs
- Discomfort in the pelvic area
Advanced prostate cancer that has spread to your bones can cause:
- Bone pain that doesn't go away
- Bone fractures
- Compression of the spine
While with most cancers, early detection increases the chance of a cure; it is unclear whether screening for prostate cancer reduces the number of deaths from this disease. Despite the controversy, it is still recommended that men undergo annual screening for this disease utilizing digital rectal examination (DRE), PSA blood test or transrectal ultrasonography. Currently, it is recommended that men begin annual screening with PSA and DRE at age 50 and that men from Afro Caribbean origin and men with a strong family history of prostate cancer begin annual screening at age 45.
The combination of detail gained by the PSA and DRE together improves the chance of identifying prostate cancer at an early stage.
- Digital Rectal Exam (DRE): During a digital rectal exam (DRE), a physician inserts a gloved finger into the rectum to assess the texture and size of the prostate. If there are any abnormalities in the texture, shape or size of your gland, you may need more tests.
- PSA Blood Test: A simple blood test allows laboratory technicians to determine PSA levels. PSA is a protein that is normally secreted and disposed of by the prostate gland. Its function is involved in liquefying sperm.
It's normal for a small amount of PSA to enter your bloodstream. However, if a higher than normal level is found, it may be an indication of prostate infection, inflammation, benign prostate enlargement, or cancer. In patients with a known diagnosis of prostate cancer, the PSA level roughly reflects the total amount of cancer. The higher the PSA level , the more likely that the cancer is advanced. - Transrectal Ultrasonography: During transrectal ultrasonography, a small probe is inserted into the rectum. The probe emits high frequency sound waves that bounce off the prostate and produce echoes. A computer uses these echoes to create a picture called a sonogram that can show abnormal areas.
- Prostate biopsy: If initial test results suggest prostate cancer, a biopsy may be recommended. To do a prostate biopsy, a small ultrasound probe is inserted into the rectum. Guided by images from the probe, a fine, spring-propelled needle retrieves several very thin sections of tissue from the prostate gland. This is done under local anaesthetic.
A pathologist who specializes in diagnosing cancer and other tissue abnormalities evaluates the samples. From those, the pathologist can tell if the tissue removed is cancerous and estimate how aggressive the cancer is.
Cancer that is removed by surgical resection or needle biopsy will be classified according to the Gleason Grading System for prostate cancer. This grading system, on a scale of 2-10, helps physicians predict how rapidly the cancer is likely to spread. The tissue samples are studied, and the cancer cells are compared with healthy prostate cells. The more the cancer cells differ from the healthy cells, the more aggressive the cancer and the more likely it is to spread quickly.
The pathologist identifies the two most aggressive types of cancer cells when assigning a grade. The most common scale used to evaluate prostate cancer cells is called a Gleason score. Based on the microscopic appearance of cells, individual ratings from 1 to 5 are assigned to the two most common cancer patterns identified. These two numbers are then added together to determine your overall score. Scoring can range from 2 (nonaggressive cancer) to 10 (very aggressive cancer).
Generally, higher Gleason scores are associated with more advanced and more rapidly growing cancers than lower scores.
Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body.
Normally, cells grow and divide to form new cells as the body needs them. When cells grow old, they die, and new cells take their place.
Sometimes this orderly process goes wrong. New cells form when the body does not need them, and old cells do not die when they should. These extra cells can form a mass of tissue called a growth or tumour.
Tumours can be benign( non cancerous) or malignant ( cancerous)
Prostate cancer occurs when the cells in the prostate gland grow out of control. When cells grow out of control, they initially spread within the prostate and then grow through the capsule that covers the prostate into neighboring organs, or break away and spread through the bloodstream and lymphatic system to other parts of the body. Prostate cancer can be relatively harmless or extremely aggressive. Some prostate cancers are slow growing, causing few clinical symptoms. In these cases, a patient will often die with prostate cancer rather than from prostate cancer. Aggressive cancers spread rapidly to the lymph nodes, other organs and especially, bone.
Risk factors for prostate cancer
The chance of an individual developing cancer depends on both genetic and non-genetic factors. A genetic factor is an inherited, unchangeable trait, while a non-genetic factor is a variable in a person's environment, which can often be changed.
Non-genetic factors may include diet, exercise, or exposure to other substances present in our surroundings. These non-genetic factors are often referred to as environmental factors. Some non-genetic factors play a role in facilitating the process of healthy cells turning cancerous (i.e. the correlation between smoking and lung cancer).
Other cancers have no known environmental correlation but are known to have a genetic predisposition. A genetic predisposition means that a person may be at higher risk for a certain cancer if a family member has that type of cancer.
Hereditary or genetic factors
Researchers have estimated that approximately 9% of prostate cancers may be the result of heritable susceptibility genes. Approximately 15% of men with prostate cancer have a first-degree male relative (father or brother) with prostate cancer, compared with 8% of the general population.
Researchers have found that there are 4 alterations or mutations of the Hereditary Prostate Cancer 2 (HPC2) gene. These place men at an increased risk of developing prostate cancer. Two of these alterations result in a 5 to 10 times higher risk of prostate cancer, while the other two result in1.5 to 3 times higher risk of prostate cancer.
Researchers are unsure why one man will develop prostate cancer and another will not. Interestingly, when people from areas with low prostate cancer rates move to areas with higher prostate cancer rates, they assume the rates of their new environment, although their genetic make-up clearly has not changed. This suggests that environmental factors may play a larger role than genetic factors in the development of prostate cancer.
Age: The incidence of prostate cancer increases dramatically with increasing age. It is unusual for prostate cancer to occur in men under the age of 50. Prostate cancer is most common in men over the age of 55, with the average age at diagnosis being 70. The risk of prostate cancer increases exponentially after age 50. In fact, by the age of 60, as many 34% of men show early evidence of prostate cancer, whereas 70% of men in their 80s have the disease.
Diet: There is increasing evidence that diet plays a role in the development of prostate cancer. Some studies indicate that prostate cancer is more prevalent in populations that consume a diet high in animal fat and/or lacking certain nutrients. Many studies indicate that a higher dietary fat intake is related to a higher risk for prostate cancer. In Asian countries where more fish, vegetables, and soy products are eaten, the incidence and death rate from prostate cancer is less than in Western countries.
Lycopenes (antioxidants in tomatoes, pink grape fruit, watermelon); vitamin E (green leafy vegetables and whole grains); selenium (seafood and whole grain) may lower cancer risk.
Hormones: Some research indicates that high testosterone levels may increase the risk of prostate cancer.
Race: Prostate cancer rates are highest among blacks, intermediate among whites and lowest among native Japanese and Native Americans. Black men are nearly twice as likely to develop prostate cancer as white men and are twice as likely to die from the disease.
Factors not likely to present risk: there have been many attempts to link the following with prostate cancer, but there has been little evidence to support this.
- Vasectomy
- smoking
- sexual activity viruses
- Sexually transmitted disease.






