Smart insulin and new hope for type-1 diabetes
-
A new smart insulin could improve the lives of people with type-1 diabetes
-
The smart insulin is easier, faster, and more effective than current therapies
-
The new compound automatically activates in response to rising blood sugar
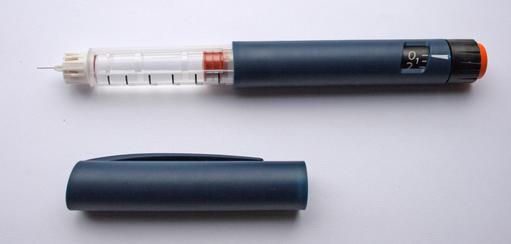
A new compound, Ins-PBA-F, referred to as ‘smart insulin’, could spare people living with type-1 diabetes the burden of frequently injecting, and constantly monitoring their blood sugar levels.
The new compound, developed by scientists from the University of Utah, USA, and reported in a 2015 edition of the Proceedings of the National Academy of Science, automatically activates when your blood sugar level soars, brings it back to normal, and remains in circulation for up to 24 hours. In the future, people with type-1 diabetes could inject the smart insulin once a day, or even less frequently, overcoming the need for constant self-monitoring, and insulin top-ups after meals.
Easier, faster and more effective
Researchers suggest that the speed, and chemical reactions of Ins-PBA-F normalizing blood sugar in diabetic mice is the same as in healthy mice responding to blood sugar changes with their own insulin. Ins-PBA-F could give a faster, more effective response to lowering blood sugar than the current long-acting insulin drug, and could be tested in humans in two to five years.
Type-1 diabetes
According to the WHO, in 2014, 9% of all adults have diabetes, and an estimated 10% of these have type-1 diabetes, a significant proportion of which are children. Type-1 diabetes is an autoimmune disease in which the body kills off all its pancreatic beta cells, which produce insulin that regulates blood sugar. Without beta cells, the body’s sugar levels fluctuate wildly. Dr Sufyan Hussain, Senior Lecturer in Diabetes, Endocrinology and Metabolism at Imperial College, London, describes type-1 diabetes:

Unrelenting regimen
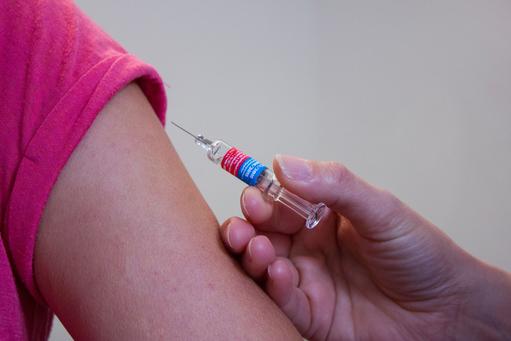
While insulin injections or infusion allow a person with type-1 diabetes to stay alive, and lead a full and active life, they neither cure the disease, nor necessarily prevent the possibility of the disease’s serious effects, which may include: kidney failure, blindness, nerve damage, heart attack, stroke and pregnancy complications. Traditional insulin therapies are a constant management challenge. Patients must carefully balance insulin doses with eating and other activities multiple times a day and night. Hussain describes the genesis, and benefits of insulin therapy:

Advantages of ‘smart insulin’
Without insulin, the body has no mechanism for moving sugar out of the blood and into cells, where it is used for energy. People with type-1 diabetes are completely dependent on their daily insulin injections for their survival, and have to check their blood-glucose level by pricking their fingers several times a day to assess how much insulin to inject. Any lapse or miscalculation in this unrelenting regimen can run the risk of dangerous high and low blood-glucose levels; both of which can be life threatening.
“In theory, with Ins-PBA-F there would be none of these glucose problems,” said co-author Dr Danny Chou, “A smart insulin drug that automatically activates in response to rising blood sugar would get rid of the need for top-up injections of insulin, and eliminate the danger of incorrect dosing”.
Takeaways
Ins-PBA-F closely mimics the way bodies return their blood sugar levels to normal after eating. According to Chou, “This is an important advance in insulin therapy. Diabetic patients still need to guess to some extent how much insulin they need. With Ins-PBA-F you would just inject it, and it wouldn’t matter if you overshot because its activity would stop when glucose levels get too low. Our smart insulin derivative appears to control blood sugar better than anything that is available to diabetes patients right now.”
|