- Each year cancer kills 8m people worldwide and cost billions
- 40% of cancer deaths could be prevented by early detection
- Nearly half of all cancer sufferers are diagnosed late when the tumors have already spread
- Victims and doctors often miss early warning signs of cancer
- Traditional tissue biopsies used to diagnose cancer are invasive, slow, costly, and often yield insufficient tissue
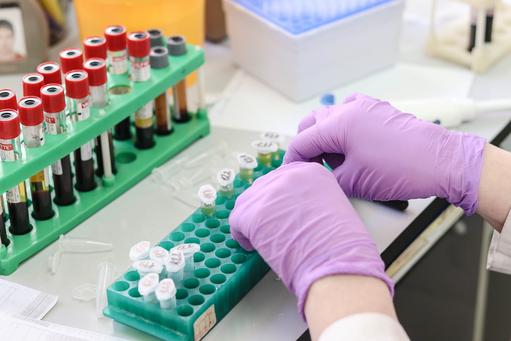
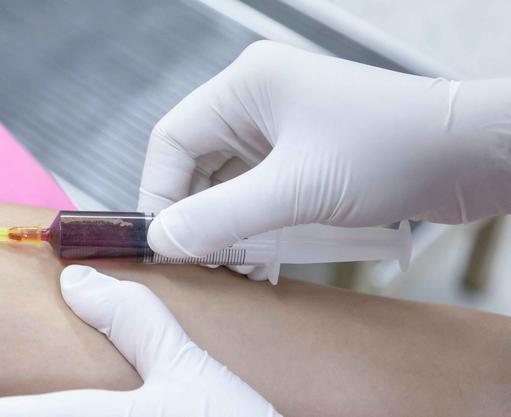
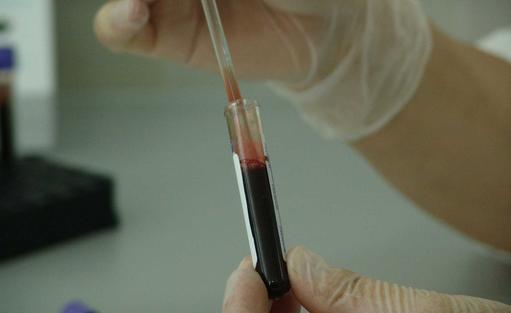
- New blood tests are being devised that simultaneously detect cancer early and inform where the cancer is in the body
- Such tests - liquid biopsies - are positioned to end the late diagnosis of cancer
- But before liquid biopsies become common practice they need to overcome a number of significant challenges
World’s first blood tests that detect and locate cancer
Just as there is a global race among immunotherapists to enhance cancer treatment, so there is a parallel race among bioengineers to speed up and improve the detection of cancer. Such races are important because nearly half of all cancer sufferers are diagnosed late, when their tumors have already metastasized: 30% to 40% of cancer deaths could be prevented by early detection and treatment.
Here we describe advances in blood tests - “liquid biopsies” - which can simultaneously detect cancer early, and identify its tissue of origin. We also, describe the growing commercialization of the technology, and some significant hurdles it still has to be overcome.
A costly killer disease
Each year cancer kills more than 8m people worldwide, 0.6m in the US and nearly 0.17m in the UK. Survival rates for pancreatic, liver, lung, ovarian, stomach, uterine and oesophageal cancers are particularly low. A large proportion of people do not know they have cancer, and many primary care doctors fail to detect its early warning signs. According to The Journal of Clinical Oncology, a staggering 44% of some types of cancers are misdiagnosed. A significant proportion of people discover that they have cancer only after presenting a different condition at A&E. Each year, the total cost of cancer to the UK’s exchequer is nearly £20bn. In the US, national spending on cancer is expected to reach US$156bn by 2020. And as populations age so some cancer prevalence rates increase, despite substantial endeavours to reduce the burden of the disease.
The UK: a stereotypical case
The UK is indicative of what is happening elsewhere in the developed world with regard to cancer diagnosis and treatment. Epidemiological trends suggest that although progress is being made to fight the disease, much work is still required. Death rates for a number of individual cancer types have declined, but rates for a few cancers have increased.
Recently, the UK’s Department of Health invested £450m to improve diagnosis, including giving primary care doctors better access to tests such as CT and MRI scans. But each year there are still some 0.17m cancer deaths in the UK, and 1 in 4 British cancer patients are unlikely to live longer than 6 months after diagnosis because they and their doctors have missed early signs of the disease. For example, in the UK only 23% of lung cancer cases are diagnosed early, as are 32% of cases of non-Hodgkin lymphoma, and 44% of ovarian cancer.
Not only does late detection increase morbidity and mortality, it significantly increases treatment costs. According to the UK’s NHS National Intelligence Network, a case of ovarian cancer detected early costs an average of £5,000 to treat, whereas one detected late at stage three or four costs £15,000. Similarly, a colon cancer patient detected early typically costs £3,000, while one not identified until a later stage would cost some £13,000.
Traditional tissue biopsies
Currently, oncologists look to pathologists for assistance in tumor diagnosis. Indeed, oncologists cannot proceed with therapy without a tissue diagnosis, nor are they able to discuss prognosis with the patient. After detecting a tumor through a physical examination or imaging, doctors use traditional tissue biopsies to gather information on the attributes of a patient’s cancer.
These pinpoint a cancer’s mutations and malignancy, but solid tissue biopsies are not always straightforward. While some cancers are easily accessed, others are hidden deep inside the body or buried in critical organs. Beyond the physical challenge, sampling from such tumors can be dangerous to patients, and once achieved, they do not always inform on current tumor dynamics. Further, traditional solid tissue biopsies are costly and time consuming to perform; they can yield insufficient tissue to obtain a good understanding of the tumor, and they can be hampered by a patient’s comorbidities, and lack of compliance.
Two significant studies
Although solid tumor tissue is still the gold standard source for clinical molecular analyses, cancer-derived material circulating in the bloodstream has become an appealing alternative showing potential to overcome some of the challenges of solid tissue biopsies.
Findings of two significant studies of liquid biopsies published in 2017 promise a more effective and patient-friendly method for diagnosing cancer: one in the journal Genome Biology, and the other in the journal Nature Genetics. Both studies are on the cusp of developing the world’s first simple blood test, which can both detect early stage cancer, and identify where in the body the cancer is located. .
The Genome Biology study
The study, reported in Genome Biology, describes findings of a blood test, referred to as the CancerLocator, which has been developed by Jasmine Zhou, Professor of Biological and Computer Sciences and her team at the University of California, Los Angeles (UCLA). The Locator detected early stage cancer in 80% of breast, lung and liver cases.
Zhou and her colleagues devised a computer program that uses genetic data to detect circulating tumor DNA (ctDNA) in blood samples. Once identified, the ctDNA is compared to a database of genetic information from hundreds of people to identify where the tumor is located. Zhou’s team discovered that tumors, which arise in different parts of the body, have different signatures, which a computer can spot. “The technology is in its infancy and requires further validation, but the potential benefits to patients are huge . . . . . Non-invasive diagnosis of cancer is important, as it allows the early detection of cancer, and the earlier the cancer is caught, the higher chance a patient has of beating the disease,” says Zhou.
The Nature Genetics study
Researchers led by Kun Zhang, Professor of Bioengineering at the University of California, San Diego (UCSD), are responsible for the study published in the journal Nature Genetics. Zhang developed a test that examined ctDNA in blood from cancer patients and, like Zhou, discovered that not only could it detect cancer early, but could also locate where the tumor is growing in the body. When a tumor starts to take over a part of the body, it competes with normal cells for nutrients and space, killing them off in the process. As normal cells die, they release their DNA into the bloodstream; and that DNA can identify the affected tissue.
“There are many technical differences on how each approach works . . . The work by the UCLA group is a computer program that uses data published previously by other groups, and has reduced the cancer detection error from roughly 60% to 26.5%. In contrast, we developed a new theoretical framework, generated our own data from over 100 patients and healthy people, and our accuracy of locating cancer in an organ is around 90%,” says Zhang, but he adds, “Major medical challenges don’t get solved by one team working alone”.
Confluence and advances in computing and biology
The research endeavors of Professors Zhou and Zhang have been made possible by the confluence and advances in computing and molecular biology. Over the past 20 years, there has been a paradigm shift in biology, a substantial increase in computing power, huge advances in artificial intelligence (AI), and the costs of data storage have plummeted. It took 13 years, US$3bn, and help from 7 governments to produce the first map of the human genome, which was completed in 2003. Soon it will be possible to sequence an entire genome in less than an hour for US$100.
The end of traditional in vitro diagnostics
Liquid biopsies are a sequencing-based technology used to detect microscopic fragments of DNA in just a few drops of blood, and hold out the potential to diagnose cancers before the onset of symptoms. Roger Kornberg, Professor of Structural Biology at Stanford University, and 2006 Nobel Laureate for Chemistry for his work in understanding how DNA is converted into RNA, “which gives a voice to genetic information that, on its own, is silent,” describes how advances in molecular science are fueling the replacement of traditional in vitro diagnostics with virtually instantaneous, point-of-care diagnostics without resort to complex processes or elaborate and expensive infrastructure. Liquid biopsies, such as those developed by Zhou and Zhang, have the potential to provide clinicians with a rapid and cheap means to detect cancer early, thereby enabling immediate treatment closely tailored to each patient’s disease state.
FDA approval of liquid biopsy
In 2016, the US Food and Drug Administration (FDA) granted Swiss pharmaceutical and biotech firm Roche approval for a liquid biopsy, which can detect gene mutations in the most common type of lung cancer, and thereby predict whether certain types of drugs can help treat it.
The clinical implementations of such a test are not widespread, and there has been no regulatory approval of liquid biopsies for diagnosing cancer generally. Notwithstanding, ctDNA is now being extensively studied, as it is a non-invasive “real-time” biomarker that can provide diagnostic and prognostic information before and during treatment; and at progression.
cfDNA and ctDNA
Cell-free DNA (cfDNA) is a broad term that describes DNA, which is freely circulating in the bloodstream, but does not necessarily originate from a tumor. Circulating tumor DNA (ctDNA) is fragmented DNA, which is derived directly from a tumor or from circulating tumor cells (CTCs).
Commercialization of the liquid biopsy race
Bill Gates, Jeff Bezos and leading venture capitalists have poured hundreds of millions into the goal of developing liquid biopsies. The US market alone is projected at US$29bn, according to a 2015 report from investment bank Piper Jaffray. Currently, there are about 40 companies in the US analyzing blood for fragments of DNA shed by dying cancer cells. Notwithstanding, only a few companies have successfully marketed liquid biopsies, and these are limited to identifying the best treatments for certain cancers, and to update treatments as the cancer mutates. So far, no one has been successful in diagnosing incipient cancer from a vial of blood drawn from a patient who looks and feels perfectly healthy.
Some US companies in the liquid biopsy race
At the 2016 meeting of the American Society of Clinical Oncology (ASCO), a Silicon Valley start-up, Guardant Health, which has raised some US$200m, presented findings from a large study involving over 15,000 participants, which demonstrated the accuracy of its liquid biopsy test, Guardant360, for patients with advanced solid tumors. The study found the same patterns of genomic changes in cfDNA reported by the Guardant360 test as those found in 398 patients with matching tissue samples between 94% and 100% of the time.
The 70-gene test is the first comprehensive, non-invasive genomic cancer-sequencing test to market, and according to the company, about 2,000 physicians worldwide have used it. Guardant expects to continue to develop its technology, and maintain a commercial lead in the cfDNA liquid biopsy space. The next step for Guardant is to go beyond sequencing, which matches patients to targeted oncology drugs to the early detection of cancer itself.
Also in 2016 Gates and Bezos teamed up with San Diego's Illumina, which makes most of the DNA sequencing machines that pick appropriate treatments for cancer patients, to launch another liquid biopsy start-up called Grail. In 2017, Grail raised US$900m to help it develop blood-based diagnostics to enable routine, early detection of cancer. The company aims to refine and validate its liquid biopsy technology by running a number of large-scale clinical studies where it expects to sequence hundreds of thousands of patients. Another Californian-based biotech start-up, Freemome, raised US$65m to validate its liquid biopsy technology for the early detection of cancer.
Takeaways
Despite findings of the two 2017 studies reported in the journals Genome Biology and Nature genetics, FDA approval of Roche’s liquid biopsy, massive increase in investment, and significant commercial biotech activity, there is a gap between reality and aspirations for liquid biopsies. To provide doctors with a reliable, point-of-care means to detect cancer early, liquid biopsies will have to overcome several significant challenges. The major one is assay sensitivity and specificity for analysis of ctDNA and cfDNA. To compete with the gold standard solid tissue biopsy, and to ensure that patients receive early diagnosis and appropriate treatment, a successful liquid biopsy assay will have to demonstrate a high positive predictive value. Concomitantly, good sensitivity and excellent specificity will be required to yield acceptable rates of false positives and false negatives. Notwithstanding, the race among bioengineers to develop a non-invasive “real-time” liquid biopsy to detect cancer early is gaining momentum.
|