Tag
Tagged: commentary
Directory:
Tags:
|
|
|
Directory:
Tags:

|
|
|
Directory:
Tags:

|
Directory:
Tags:

|
|
|
Directory:
Tags:
|
|
|
Directory:
Tags:
- A new gene editing study is poised on the cusp of medical history because it holds out the prospect of providing a cure for hemophilia
- Hemophilia is a rare incurable life-threatening blood disorder
- People with hemophilia have little or no protein needed for normal blood clotting
- Severe forms of the disorder may result in spontaneous and excessive bleeding
- In recent history many people with hemophilia died before they reached adulthood because of the dearth of effective treatments
- A breakthrough therapy in the 1980s was contaminated with deadly viruses
A cure for hemophilia?
A study led by researchers from Barts Health NHS Trust and Queen Mary University London and published in a 2017 edition of the New England Journal of Medicine has made a significant step forward towards finding a cure for hemophilia A, a rare incurable life threatening-blood disorder, which is caused by the failure to produce certain proteins required for blood clotting. In recent history only a few people with hemophilia survived into adulthood. This was because of the dearth of effective treatments and any small cut or internal hemorrhaging after even a minor bruise was often fatal.
The royal disease
There are 2 main types of hemophilia: A and B. Both are rare congenital bleeding disorders sometimes referred to as “the royal disease,” because in the 19th and 20th centuries hemophilia affected European royal families. Queen Victoria of England is believed to have been a carrier of hemophilia B, a rarer condition than hemophilia A. 2 of Victoria’s 5 daughters (Alice and Beatrice) were also carriers. Through marriage they passed on the mutation to various royal houses across Europe including those of Germany, Russia and Spain. Victoria’s son Prince Leopold was diagnosed with hemophilia A when he was a child. He died at 31 and throughout his life had a constant staff of doctors around him.
Epidemiology
The worldwide incidence of hemophilia A is about 1 in 5,000 males, with approximately 33% of affected individuals not having a family history of the disorder, which in their cases result from a new mutation or an acquired immunologic process. Only 25% of people with hemophilia receive adequate treatment; most of these are in developed nations. In 2016 there were some 7,700 people diagnosed with the condition in the UK, 2,000 of whom had a severe form with virtually no blood clotting protein. In the US there are some 20,000 people living with the disorder. Morbidity and death from hemophilia are primarily the result of haemorrhage, although HIV and hepatitis infections became prominent in patients who received therapies with contaminated blood products prior to the mid-1980s: see below.
Etiology
Hemophilia A and B are similar disorders. Both are caused by an inherited or acquired genetic mutation, which reduces or eliminates the coagulation genes referred to as factor VIII for hemophilia A, and factor IX for hemophilia B. Factors VIII and IX are essential blood clotting proteins, which work with platelets to stop or control bleeding. The amount of the protein present in your blood and its activity determines the severity of symptoms, which range from mild to severe. Factors VIII and IX deficiencies are the best-known and most common types of hemophilia, but other clotting factor deficiencies also exist. Factors VIII and IX are encoded in genes and located on the X chromosomes, which come in pairs. Females have 2 X chromosomes, while males have 1 X and 1 Y chromosome. Only the X chromosome carries the genes related to clotting factors. A male who has a hemophilia gene on his X chromosome will have hemophilia. Since females have 2 X chromosomes, a mutation must be present in both copies of the gene to cause the hemophilia. When a female has a hemophilia gene on only 1 of her X chromosomes, she is a "carrier” of the disorder and can pass the gene to her children. Sometimes carriers have low levels of a clotting factor and therefore have symptoms of hemophilia, including bleeding.
|
|
Directory:
Tags:
- In high-income countries populations are aging
- By 2050 the world population of people over 60 is projected to reach 2bn
- Age-related low back pain is the highest contributor to disability in the world
- Over 80% of people will experience back pain at some point in their life
- Older people with back pain have a higher chance of dying prematurely
- The causes of back pain are difficult to determine which presents challenges for the diagnosis and management of the condition
- The US $100bn-a-year American back pain industry is “ineffective”
- Each year 10,000 and 300,000 spine fusion surgeries are carried out in the UK and US respectively
- 20% of spinal fusion surgeries are undertaken without good evidence
- In 10 to 39% of spine surgery patients pain continues or worsens after surgeries
Age of the aged and low back pain
A triumph of 20th century medicine is that it has created the “age of the aged”. By 2050 the world population of people aged 60 and older is projected to be 2bn, up from 900m in 2015. Today, there are 125m people aged 80 and older and by 2050 there is expected to be 434m people in this age group worldwide. The average age of the UK population has reached 40. Some 22% will be over 65 by 2031, and this will exceed the percentage of the UK population under 25. 33% of people born today in the UK can expect to live to 100. However, this medical success is the source of rapidly increasing age-related disorders, which present significant challenges for the UK and other high-income nations. Low back pain (LBP) is the most common age-related pain disorder, and ranked as the highest contributor to disability in the world.
At some point back pain affects 84% of all adults in developed economies. Research published in 2017 in the journal Scoliosis Spinal Disorders suggests that LBP is the most common health problem among older adults that results in pain and disability. The over 65s are the second most common age group to seek medical advice for LBP, which represents a significant and increasing workload for health providers. Each year back pain costs the UK and US Exchequers respectively some £5bn and more than US635bn in medical treatment and lost productivity. LBP accounts for 11% of the total disability of the respective populations. This Commentary discusses therapies for LBP, and describes the changing management landscape for this vast and rapidly growing condition.
Your spine and LBP
Your spine, which supports your back, consists of 24 vertebrae, bones stacked on top of one another. At the bottom of your spine and below your vertebrae are the bones of your sacrum and coccyx. Threading through the entire length of your vertebrae is your spinal cord, which transmits signals from your brain to the rest of your body. Your spinal cord ends in your lower back, and continues as a series of nerves, which resemble a horse’s tail, hence its medical name, ‘cauda equine’. Between each vertebra are discs. In younger people discs contain a high degree of water. This gives them the ability to act like shock absorbers. During the normal aging process discs lose much of their water content and degenerate. Such degenerative spinal structures may result in a herniated disc when the disc nucleus extrudes through the disc’s outer fibres, or a compression of nerve roots, which may lead to radiculopathy. This is a condition more commonly known as sciatica, which is pain caused by compression of a spinal nerve root in the lower back that is often associated with the degeneration of an intervertebral disc, and can manifest itself as pain, numbness, or weakness of the buttock and outer side of the leg.
Challenges in diagnosis
Because your back is comprised of so many connected tissues, which include bones, muscles, ligaments, nerves, tendons, and joints, it is often difficult for doctors to say with confidence what causes back pain even with the help of X-rays and MRI scans. Usually, LBP does not have a serious cause. In the majority of cases LBP will reduce and often disappear within 4 to 6 weeks, and therefore can be self-managed by keeping mobile and taking over-the-counter painkillers. However, in a relatively small proportion of people with LBP, the pain and disability can persist for many months or even years. Once LBP has been present for more than a year few people return to normal activities. There is not sufficient evidence to suggest definitive management pathways for this group that accounts for the majority of the health and social costs associated with LBP.
Assessing treatment options for back pain
Ranjeev Bhangoo, a consultant neurosurgeon at Kings’ College Hospital Trust, London, and the London Neurosurgery Partnership describes the nature and role of intervertebral discs and how treatment options should be assessed.
“When a person presents with a problem in the lower back, which might manifest as leg or arm pain, you need to ask 3 questions: (i) is the history of the pain compatible with a particular disc causing the problem? (ii) Does an examination suggest that a particular disc is causing a problem? And (iii) does a scan show that the disc you thought was the problem is the problem? If all 3 answers align, then there maybe some good reason to consider treatment options. If the 3 answers are not aligned, be weary of a surgeon suggesting intervention because 90% of us will experience back pain at some point in our lives, and 90% of the population don’t need back surgery.”
Back pain requiring immediate medical attention
Although the majority of LBP tends to be benign and temporary, people should seek immediate medical advice if their back pain is associated with certain red flags such as loss of bladder control; loss of weight, fever, upper back or chest pain; or if there is no obvious cause for the pain; or if the pain is accompanied by weakness, loss of sensation or persistent pins and needles in the lower limbs. Also, people with chronic lifetime conditions such as cancer should pay particular attention to back pain.
Epidemiology of LBP
Back pain affects approximately 700m people worldwide. A 2011 report by the US Institute of Medicine, estimates that 100m Americans are living with chronic back pain, which is more than the total affected by heart disease, cancer, and diabetes combined. This represents a vast market for therapies that include surgery and the prescription of opioids. Estimates of the prevalence of LBP vary significantly between studies. There is no convincing evidence that age affects the prevalence of back pain, and published data do not distinguish between LBP that persists for more than, or less than, a year. Each year LBP affects some 33% of UK adults, and around 20% of these - about 2.8m - will consult their GP. One year after a first episode of back pain, 62% of people still experience pain, and 16% of those initially unable to work are not working after 1 year. Typically in about 60% of cases pain and disability improve rapidly during the first month after onset.
|
|
Directory:
Tags:

- Everyone connected with healthcare supports interoperability saying it improves care, reduces medical errors and lowers costs
- But interoperability is a long way from reality and electronic patient records are only part of an answer
- Could Blockchain a technology disrupting financial systems resolve interoperability in healthcare?
- Blockchain is an open-source decentralized “accounting” platform that underpins crypto currencies
- Blockchain does not require any central data hubs, which in healthcare have been shown to be easily breached
- Blockchain technology creates a virtual digital ledger that could automatically record every interaction with patient data in a cryptographically verifiable manner
- Some experts believe that Blockchain could improve diagnosis, enhance personalised therapies, and prevent highly prevalent devastating and costly diseases
- Why aren’t healthcare leaders pursuing Blockchain with vigour?
Why Blockchain technology will not disrupt healthcare
Blockchain technology is disrupting financial systems by enhancing the reconciliation of global transactions and creating an immutable audit trail, which significantly enhances the ability to track information at lower costs, while protecting confidentiality. Could Blockchain do something similar for healthcare and resolve the challenges of interoperability by providing an inexpensive and enhanced means to immutably track, store, and protect a variety of patient data from multiple sources, while giving different levels of access to health professionals and the public?
Blockchain and crypto currencies
You might not have heard of Blockchain, but probably you have heard of bitcoin; an intangible or crypto currency, which was created in 2008 when a programmer called Satoshi Nakamoto (a pseudonym) described bitcoin’s design in a paper posted to a cryptography e-mail list. Then in early 2009 Nakamoto released Blockchain: an open source, global decentralized accounting ledger, which underpins bitcoin by executing and immutably recording transactions without the need of a middleman. Instead of a centrally managed database, copies of the cryptographic balance book are spread across a network and automatically updated as transactions take place. Bitcoin gave rise to other crypto-currencies. Crypto currencies only exist as transactions and balances recorded on a public ledger in the cloud, and verified by a distributed group of computers.
Broad support for interoperability
Just about everyone connected with healthcare - clinicians, providers, payers, patients and policy makers - support interoperability, suggesting data must flow rapidly, easily and flawlessly through healthcare ecosystems to reduce medical errors, improve diagnosis, enhance patient care, and lower costs. Despite such overwhelming support, interoperability is a long way from a reality. As a result, health providers spend too much time calling other providers about patient information, emailing images and records, and attempting to coordinate care efforts across disjointed and disconnected healthcare systems. This is a significant drain on valuable human resources, which could be more effectively spent with patients or used to remotely monitor patients’ conditions. Blockchain may provide a solution to challenges of interoperability in healthcare.
Electronic patient records do not resolve interoperability
A common misconception is that electronic patient records (EPR) resolve interoperability. They do not. EPRs were created to coordinate patient care inside healthcare settings by replacing paper records and filing cabinets. EPRs were not designed as open systems, which can easily collect, amalgamate and monitor a range of medical, genetic and personal information from multiple sources. To realize the full potential and promise of interoperability EPRs need to be easily accessible digitally, and in addition, have the capability to collect and manage remotely generated patient healthcare data as well as pharmacy and prescription information; family-health histories; genomic information and clinical-study data. To make this a reality existing data management conventions need to be significantly enhanced, and this is where Blockchain could help.
|
|
Directory:
Tags:
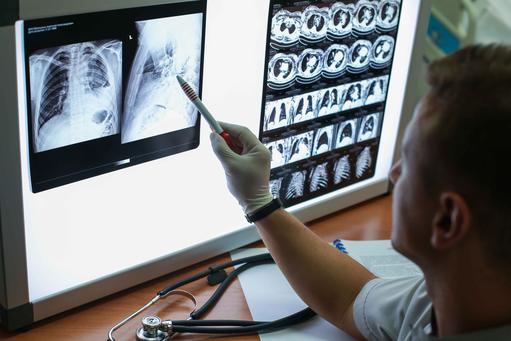
- Chronic obstructive pulmonary disease (COPD) is a lung condition, which makes it hard to breathe, but is often preventable and treatable
- COPD affects some 210m people worldwide, its prevalence is increasing, and it costs billions in treatment and lost production
- By 2020 COPD is projected to be the 3rd leading cause of death worldwide
- Recently, scientific advances have benefitted COPD research
- But COPD researchers are challenged to provide compelling data in support of their studies
- COPD research would benefit from smart online communications strategies
- This could strengthen collaboration among globally dispersed scientists and people living with COPD, and expand the geographies from which COPD data are retrieved
Chronic Obstructive Pulmonary Disease (COPD) and the battle for breath
Chronic Obstructive Pulmonary Disease (COPD) is a common, preventable and treatable disorder, which affects 210m people worldwide. Its prevalence is increasing globally, and each year it causes some 3m deaths. Although COPD therapies have improved substantially in recent years, and benefit from advancing science, researchers are still challenged to provide compelling data in support of their studies. There is no definitive treatment for COPD, and more research is needed to improve the condition’s clinical management. There are regions of the world where the prevalence of COPD is increasing significantly, but where information about the disorder is sparse. This Commentary suggests that COPD research could benefit by enhancing the connectivity of globally dispersed scientists and people living with the disorder, and expanding the geographies from where COPD data are retrieved. Before suggesting ways to achieve this, let us describe COPD, and its vast and escalating burden.
COPD is an umbrella term used to describe common progressive lifetime diseases, which damage the lungs and airways, and make breathing difficult. Its prevalence is increasing especially in developing countries. It is the 4th leading cause of death worldwide and projected to be the 3rd by 2020. The causes of COPD are well known, but the nature of the condition is still not fully understood even though COPD therapies have improved significantly in recent years. The effects of COPD are persistent and progressive, but treatment can relieve symptoms, improve quality of life and reduce the risk of death. COPD impacts people differently, medications affect patients differently, and such differences make it challenging for doctors to identify patients who are at risk of a more rapidly progressing condition.
Although COPD is complex with different etiologies, pathogens and physiological effects, there are two main forms: (i) chronic bronchitis, which involves a long-term cough with mucus, and (ii) emphysema, which involves damage to the lungs over time. COPD also has significant extra-pulmonary effects, which include weight loss, nutritional abnormalities, skeletal muscle dysfunction, and it is also a major cause of psychological suffering. Further, COPD may promote heart failure because obstruction of the airways and damage to the lining of the lungs can result in abnormally low oxygen levels in the vessels inside the lungs. This creates excess strain on the right ventricle from pulmonary hypertension, which can result in heart failure.
In developed countries, the biggest risk factor for the development of COPD is cigarette smoking, whereas indoor pollutants are the major risk factor for the disease in developing nations. Not all smokers develop COPD and the reasons for disease susceptibility in these individuals have not been fully elucidated. Although the mechanisms underlying COPD remain poorly understood, the disease is associated with chronic inflammation, which is usually corticosteroid resistant, destruction of the airways, and lung parenchyma (functional tissue). There is no cure for COPD, but it is sometimes partially reversible with the administration of inhaled long-acting bronchodilators, and its progression can be slowed through smart maintenance therapy, in particular a cessation of smoking. People with stage 1 or 2 COPD lose at most a few years of life expectancy at age 65 compared with persons with no lung disease, in addition to any years lost due to smoking. Current smokers with stage 3 or 4 COPD lose about 6 years of life expectancy, in addition to the almost 4 years lost due to smoking.
The economic burden of COPD is vast and increasing, with attributed costs for hospitalizations, loss of productivity, and disability, in addition to medical care. In 2010, the condition’s annual cost in the US alone was estimated to be approximately US$50bn, which includes $20bn in indirect costs, and $30bn in direct health care expenditures. COPD treatment costs the UK more than £1.9bn each year. Over the past decade in the UK progress in tracking the disease has stagnated, and there is a wide variation in the quality of care.
The prevalence of COPD has increased dramatically due to a combination of aging populations, higher smoking prevalence, changing lifestyles and environmental pollution. In developed economies, COPD affects an estimated 8 to 10% of the adult population, 15 to 20% of the smoking population, and 50 to 80% of lung cancer patients with substantial smoking histories. For many years, COPD was considered to be a disease of developed nations, but its prevalence is increasing significantly in developing countries, where almost 90% of COPD deaths occur. Even though most of the research data on COPD comes from developed countries, accurate epidemiologic data on the condition are challenging and expensive to collect. There is a dearth of systematically collected COPD prevalence data from developing nations, and a paucity of COPD studies in Africa, SE Asia and the Eastern Mediterranean region. Most of the available prevalence estimates from low- to middle-income countries are not based on spirometry testing (the internationally accepted gold standard for the diagnosis of COPD, which measures lung capacity). Hence, the available COPD data from developing countries cannot be interpreted reliably in a global context, and more data from these regions are necessary to extend and support further studies.
Chronic Obstructive Pulmonary Disease (COPD)
COPD is an umbrella term used to describe common progressive lifetime diseases, which damage the lungs and airways, and make breathing difficult. Its prevalence is increasing especially in developing countries. It is the 4th leading cause of death worldwide and projected to be the 3rd by 2020. The causes of COPD are well known, but the nature of the condition is still not fully understood even though COPD therapies have improved significantly in recent years. The effects of COPD are persistent and progressive, but treatment can relieve symptoms, improve quality of life and reduce the risk of death. COPD impacts people differently, medications affect patients differently, and such differences make it challenging for doctors to identify patients who are at risk of a more rapidly progressing condition.
Although COPD is complex with different etiologies, pathogens and physiological effects, there are two main forms: (i) chronic bronchitis, which involves a long-term cough with mucus, and (ii) emphysema, which involves damage to the lungs over time. COPD also has significant extra-pulmonary effects, which include weight loss, nutritional abnormalities, skeletal muscle dysfunction, and it is also a major cause of psychological suffering. Further, COPD may promote heart failure because obstruction of the airways and damage to the lining of the lungs can result in abnormally low oxygen levels in the vessels inside the lungs. This creates excess strain on the right ventricle from pulmonary hypertension, which can result in heart failure.
In developed countries, the biggest risk factor for the development of COPD is cigarette smoking, whereas indoor pollutants are the major risk factor for the disease in developing nations. Not all smokers develop COPD and the reasons for disease susceptibility in these individuals have not been fully elucidated. Although the mechanisms underlying COPD remain poorly understood, the disease is associated with chronic inflammation, which is usually corticosteroid resistant, destruction of the airways, and lung parenchyma (functional tissue). There is no cure for COPD, but it is sometimes partially reversible with the administration of inhaled long-acting bronchodilators, and its progression can be slowed through smart maintenance therapy, in particular a cessation of smoking. People with stage 1 or 2 COPD lose at most a few years of life expectancy at age 65 compared with persons with no lung disease, in addition to any years lost due to smoking. Current smokers with stage 3 or 4 COPD lose about 6 years of life expectancy, in addition to the almost 4 years lost due to smoking.
The economic burden of COPD is vast and increasing, with attributed costs for hospitalizations, loss of productivity, and disability, in addition to medical care. In 2010, the condition’s annual cost in the US alone was estimated to be approximately US$50bn, which includes $20bn in indirect costs, and $30bn in direct health care expenditures. COPD treatment costs the UK more than £1.9bn each year. Over the past decade in the UK progress in tracking the disease has stagnated, and there is a wide variation in the quality of care.
Prevalence
The prevalence of COPD has increased dramatically due to a combination of aging populations, higher smoking prevalence, changing lifestyles and environmental pollution. In developed economies, COPD affects an estimated 8 to 10% of the adult population, 15 to 20% of the smoking population, and 50 to 80% of lung cancer patients with substantial smoking histories. For many years, COPD was considered to be a disease of developed nations, but its prevalence is increasing significantly in developing countries, where almost 90% of COPD deaths occur. Even though most of the research data on COPD comes from developed countries, accurate epidemiologic data on the condition are challenging and expensive to collect. There is a dearth of systematically collected COPD prevalence data from developing nations, and a paucity of COPD studies in Africa, SE Asia and the Eastern Mediterranean region. Most of the available prevalence estimates from low- to middle-income countries are not based on spirometry testing (the internationally accepted gold standard for the diagnosis of COPD, which measures lung capacity). Hence, the available COPD data from developing countries cannot be interpreted reliably in a global context, and more data from these regions are necessary to extend and support further studies.
|
|
Directory:
Tags:
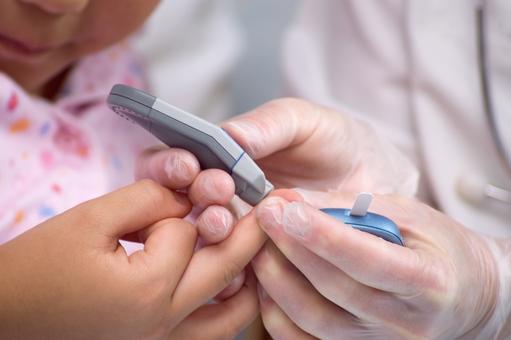
- A 2017 research project found that only 6 out of 18 FDA-approved blood glucose monitoring (BGM) systems tested were accurate
- Each day BGM systems are used by millions of people with diabetes to help them self-manage their condition, and avoid devastating and costly complications
- Thousands of similar smart devices support the prevention and self management of other chronic lifetime conditions, whose prevalence levels are high
- The increasing demand for healthcare, its escalating costs, and rapidly evolving technologies are driving the growth of such remote self-managed devices
- The most valuable aspect of such devices is the data they produce
- These data tend to be under valued and under utilized by healthcare providers
- This has created an opportunity for giant technology companies to enter the healthcare market with a plethora of smart devices and start utilizing the data they collect to enhance patient outcomes and lower costs
- Giant technology companies could dis-intermediate GPs and re-engineer primary care
Digital blood glucose monitors and the disruptive impact of giant tech companies on healthcare
A 2017 research project, which tested 18 FDA-approved digital blood glucose monitoring (BGM) systems, which are used daily by millions of people with diabetes to check the concentration of glucose in their blood, found that only 6 were accurate. The research, led by David Klonoff of the Diabetes Research Institute at San Mateo, California, was funded by Abbott Laboratories.
This Commentary describes both traditional and next-generation BGM systems, and Klonoff’s research. The Commentary suggests that BGM systems are just one part of a vast, global, rapidly growing market for consumer healthcare devices, and argues that the most valuable aspect of these devices is the data they collect. With some notable exceptions, healthcare professionals do not optimally utilize these data to enhance care and reduce costs. This has created for an opportunity for technology companies to enter the healthcare market and re-engineer primary care. The one thing, which might slow the march of giant technology companies into mainstream healthcare, is the privacy issue.
Traditional and next-generation BGM systems
Traditional BGM systems
Regularly, each day, BGM systems are used by millions of people with diabetes to help them manage their condition. Managing diabetes varies from individual to individual, and peoples with diabetes usually self-monitor their blood glucose concentration from a small drop of capillary blood taken from a finger prick. They then apply the blood to a chemically active disposable 'test-strip'. Different manufacturers use different technology, but most systems measure an electrical characteristic, and use this to determine the glucose level in the blood. Such monitoring is the most common way for a person with diabetes to understand how different foods, medications, and activities affect their condition. The challenge for individuals with diabetes is that blood glucose levels have to be tested up to 12 times a day. People obliged to do this find finger pricking painful, inconvenient and intrusive, and, as a consequence, many people with diabetes do not check their glucose levels as frequently as they should, and this can have significant health implications. If your levels drop too low, you face the threat of hypoglycemia, which can cause confusion or disorientation, and in its most severe forms, loss of consciousness, coma or even death. Conversely, if your blood glucose levels are too high over a long period, you risk heart disease, blindness, renal failure and lower limb amputation.Next generation BGM system
Abbott Laboratories Inc. markets a BGM system, which eliminates the need for routine finger pricks that are necessary when using traditional glucose monitors. Instead of finger pricks and strips, the BGM system, which measures interstitial fluid glucose levels, comprises a small sensor and a reader. An optional companion app for Android mobile devices is also available. The sensor is a few centimetres in diameter and is designed to stay in place for 10 days. It is applied to the skin, usually on the upper arm. A thin (0.4 mm), flexible and sterile fibre within the sensor is inserted in the skin to a depth of 5 mm. The fibre draws interstitial fluid from the muscle into the sensor, where glucose levels are automatically measured every minute and stored at 15-minute intervals for 8 hours. Glucose levels can be seen at any time by scanning the reader over the sensor. When scanned the sensor provides an answer immediately. It also shows an 8-hour history of your blood glucose levels, and a trend arrow showing the direction your glucose is heading. The device avoids the pain, and inconvenience caused by finger-prick sampling, which can deter people with diabetes from taking regular measurements. In the UK the system costs £58 for the reader, plus £58 for a disposable sensor, which must be replaced every 10 days and from November 2017 have been available on the NHS. Abbott Laboratories is a global NASDAQ traded US MedTech Company, with a market cap of US$86bn; annual revenues of US$21bn, and a diabetes care division, which produces annual revenues of some US$600m.
Klonoff’s research on BGM systems
BGM systems used by Klonoff and his team for their research were acquired over-the-counter and independent of their manufacturers. All were tested according to a protocol developed by a panel of experts in BGM surveillance testing.
Klonoff’s research specified that for a BGM system to be compliant, a blood glucose value must be within 15% of a reference plasma value for a blood glucose >100 mg/dl, and within 15 mg/dl of a reference plasma value for a blood glucose approved” a BGM system had to pass all 3 trials. Only 6 out of 18 passed by achieving an overall compliance rate of 95% or higher.
|
|
















